|
Traveling is one of my greatest joys in life so when I was diagnosed with Crohn’s Disease, I refused to let my symptoms prevent me from doing what I love. Flying can be a big source of anxiety for those with Inflammatory Bowel Disease. There are many factors that can play into the feeling, but one of the most common ones is the concern about not being near a bathroom. Flying is also a necessity in some situations - work travel, family visits, etc. Your travel schedule and GI symptoms unfortunately don’t coordinate to make sure you have a comfortable experience. That being said, anything to reduce the anxiety around flying when experiencing GI symptoms is a welcome suggestion. One of the most simple ways to combat a common concern is to make sure you are positioned near a bathroom on the flight. On certain airlines, you can choose your seat ahead of time. This means locking in that prime aisle seat right next to the facilities. No stepping over other passengers mid bathroom emergency and you are close by so you won’t have to fumble down the aisle as you’re trying to make it to the facilities. This is great for airlines that offer this preselection option.This isn’t always the case, though. I most frequently fly Southwest which has open seating (i.e. no preselected seats). This has caused me a lot of anxiety over the years - panicking when I didn’t get an early boarding group, having to ask passengers to switch seats with me and awkwardly explaining why, and trying to do anything I could to avoid having to use the bathroom on flights (which was not very effective). A few years ago, I saw some fellow IBD patients share a travel tip and it instantly changed traveling for me. Southwest offers disability preboarding and Inflammatory Bowel Disease is a disability. When I first found this out, I was in the stage of denying IBD was a disability that impacted functions of my life, but now looking back I wish I would have accepted this sooner so that I could utilize the resources that are there for IBD patients. That is why they are there, to help us! I check in like I normally would for my Southwest flight and once I get to the gate, I speak with the gate attendant. I explain that I require disability boarding due to my Crohn’s Disease and need to be seated next to a bathroom. I always have my doctor’s note on hand to show if it is needed. The gate attendant updates my boarding pass to list preboarding status and I am good to go.
Disability preboarding includes passengers with all types of disabilities. This means you will often be boarding with wheelchair users and other passengers with mobility challenges. I understand that for them it is more necessary that they have the seats closer to the front of the plane, while for me I have the option of sitting near the rear bathrooms. That being said, I make sure not to take the front seats if they are needed by others. When I board the plane, I confirm with a flight attendant that there are functioning bathrooms at the back of the plane and head on back to secure my seat. This small tweak to my travel routine has made a significant impact on my anxiety level while traveling. The knowledge that I will be able to have easy access to a bathroom while in the air is a huge comfort. I recently realized how many fellow IBD patients don’t know that this is an option. I didn’t for the longest time, until I saw a patient advocate share the information ( I wish I remembered specifically who because I would definitely shout them out!). I know how much that information helped me so I want to help spread the word that Southwest does offer this option to support passengers with visible AND invisible disabilities. As I mentioned before, I went through a period where I was in denial that IBD was a disability. For a while when I started to actually utilize these types of programs, I would feel embarrassed. I thought people were looking at me strangely because they couldn’t see that I was sick. I went out of my way to awkwardly over justify why I needed certain accommodations. It has taken me years to work through and I still struggle with it, but I have gotten a lot more comfortable. Just because my condition isn’t visible doesn’t make me any less deserving of the programs that are in place to assist people like me. I am not saying to utilize every offered accommodation “just because,” but if it is something that will impact your condition, symptoms, or quality of life, you should feel empowered to use these resources that are there for you. As an IBD patient did you know that this was an option for you? How would an accommodation like this impact your travel experience with IBD? xx
0 Comments
At the beginning of my IBD journey, I had the pleasure of working with Oshi Health in their early days. At the time, they were mainly a tracking app for GI symptoms. My mom and I attended a user research group in New York and met with some of the consulting physicians. This was the first time I was introduced to the concept of integrative care. It wasn’t something that was a reality yet for many patients, but the idea that providers could work together and treat the whole person was a positive one.
Almost 5 years later, I had the pleasure of sitting down with Michael Currier, a GI Physician Associate at Oshi Health, to get an update on how the company and the app have evolved. Oshi Health has grown from a tracking app for GI conditions to a full service option for receiving integrative GI care. Through the app, you are matched with an Oshi GI provider who you see virtually. The appointments are on average around 45-minutes as opposed to the usual in office 10-15 minutes that are standard practice for most of us. Your provider gets to really know you and dig into the whole story your body and symptoms are telling. They can order labs or diagnostic procedures for you with their local partners (they have a scheduling team that takes care of this for you!), and you are matched with an entire team of providers at Oshi. They understand that the best GI care is multifaceted and consideration needs to be given to the effects both diet and mental health have on GI conditions. Through Oshi, you are paired with a Registered Dietician and a GI Psychologist to help you feel better from all angles. The best part, in my opinion, is that your GI provider, dietician, and psychologist all work together behind the scenes to collaborate on the best care plan for you.
A few other highlights for me are: they will work with a doctor you are already seeing if you want additional support, but aren’t ready to make a complete switch and you have access to your Oshi team via chat so you never are without a line of support. Another important call out is that they partner with many insurance companies that will cover your care through Oshi.
On an individual level, Oshi Health is changing the game for patients. They are breaking down barriers of accessibility when it comes to GI care. They are empowering patients by treating them as a whole person, not just patients. This is also revolutionary for our healthcare system in general. It is rare that there is so much collaboration between different providers despite how much of a positive impact it could make. Oshi Health has designed a model that flips that statement on its head and is challenging what we currently accept as the status quo. You can listen to my conversation with Michael Currier from Oshi Health on this week’s episode of Crohnically Mom. He explains more about the benefits of integrative care, how Oshi is creating more accessible GI care, and how their model gets patients better. One of my favorite sessions at DDW focused on pediatric IBD. This is a topic that is near and dear to my heart as members of my family have been diagnosed with IBD in childhood and I know my own children are at a greater risk. Nisha Thacker, an Accredited Practicing Dietician at Sydney Children’s Hospitals Network in Australia, presented her team’s findings, which provided some very valuable insight into pediatric IBD risk factors, but also left me with some questions. I am going to share some slides with key takeaways I gained from the presentation and share my thoughts on the findings from the perspective of a patient and a mom. A few background pieces of information that were shared prior to reviewing the findings were:
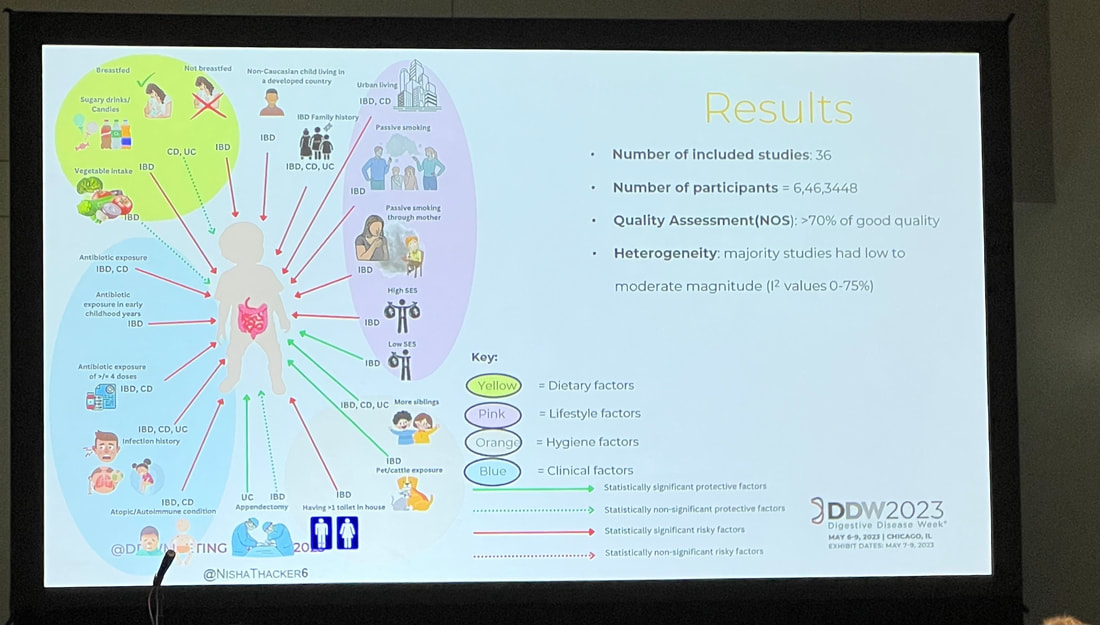
Nisha shared a diagram mapping out the influence of dietary, lifestyle, hygiene, and clinical factors and their effect on pediatric IBD risk, which I share below. Many of the factors that have a negative impact on IBD risk are commonplace in our Western society. Western diet in general is a risk factor, but there are a lot of factors that paint the picture of middle class or upper class Western life. Things like having more than one toilet in a home, urban living, and early antibiotic exposure are all contributing risk factors. On the other hand, having more siblings, being exposed to pets or cattle, and not being formula fed are all contributing factors to lower IBD risk. I thought the most telling though, was that a non-Caucasian child living in a developed country has a higher risk of developing IBD. You can’t review this information without thinking to yourself that maybe we are doing something wrong here in the West. In other cultures, there is a greater focus on holistic treatments instead of jumping straight to antibiotics. There are larger, generational households with more children. Mothers have more family and societal support postpartum, which encourages successful breastfeeding. There is less consumption of sugary or processed foods, and really a different dietary structure. Our lifestyle in the West does not bode well for avoiding the development of IBD. One of the things that really struck me about these findings was the impact that not breastfeeding has as a risk factor for IBD. I found this interesting because this is identified as a negative factor in other pediatric and maternal health outcomes. If we know that supporting a mother to breastfeed will influence pediatric outcomes then why don’t we have more support? Why do we not have adequate maternity leave to support breastfeeding mothers? Why do we not have healthcare coverage that universally provides continued lactation support? I would love to see a study on IBD rates in countries with longer maternity leave or countries with higher breastfeeding rates. This also speaks to parental support as a whole. Western culture does not champion multigenerational households like other countries and cultures do. With multigenerational households come additional people to help – whether that be in watching older children so a mother can breastfeed, preparing homemade meals for the family, or having more adults contributing to a family’s income so maybe a mother can stay home with her newborn longer. This isn’t always the case, but I think it could be worth diving into. The biggest takeaways I have as a parent are what I can do to lower the risk of IBD for my children. There are things I can’t change, like genetics or the fact that my children had to be at least partially formula fed, but there are things I can do that can make a difference.
Pet exposure is a big one that is actionable. I am working to get more information on the science behind this, but unrelated to IBD our pediatrician has mentioned the benefit of having a dog in building stronger immunity as a child. I am putting a pin in this and I hope to come back with more information. The other two easily actionable factors are diet (higher consumption of vegetables, lower consumption of sugar/candy) and antibiotic exposure. To be clear here, I believe that antibiotics are necessary in some cases and can save lives. The recommendation isn’t to never expose your child to antibiotics, it is to expose them only necessarily. The same goes for diet. This study won’t motivate me to never let my kids have cupcakes again, but it will encourage me to continue packing their diets with vegetables any chance I get. I do want to address the factors that we can’t control or we choose not to. “Mom guilt” rang in the back of my mind during this whole presentation. When I originally posted these slides on my Instagram, I received countless messages of moms freaking out. It is our nature to want to do whatever we can to protect our children, but some things truly are out of our control. I wanted to call out a few things in particular. Low socioeconomic status is an identified “protective factor” in avoiding IBD, but has many other potentially negative effects on a family. This study is viewing that data in a bubble as opposed to the whole impact of low socioeconomic status. Having more than two siblings is another “protecting factor” in IBD development. This again is something that is being looked at in a bubble. There is no recommendation to have more children for the sole purpose of protecting against IBD. The same goes for other factors such as urban living. There are some benefits in other regards when it comes to urban living. We can’t just change where we live to hopefully avoid IBD. As a mom to two little ones, there are two factors that give me a pit in my stomach. One is the risk factor of not being breastfed and the other is early life antibiotic exposure. Breastfeeding is something that is so deeply personal and challenging. Sometimes there are medical reasons (physical or mental) that prevent breastfeeding. Other times mothers are not able to breastfeed due to lack of resources or support. There are also scenarios where breastfeeding is not an option at all. This is such a complex issue and emotionally charged on both sides. As a mom, if you read this and get a pit in your stomach, try to remember that this information is again, in a bubble. Just because you didn’t breastfeed does not mean your child will have IBD. The same goes for early antibiotic usage. This is something that can be out of a parent’s control. If a baby has an infection that needs to be treated with antibiotics, that is the best course of action. There are situations where the benefit outweighs the risk and there is nothing that can change that. In conclusion, this session provided some very interesting insight and shared some low risk lifestyle changes that we can adapt to help lower our children’s risk of IBD. On the other hand, I am curious to see additional studies that evaluate these factors on the basis of risk/benefit. I also am interested to see how the findings may change if the study was conducted outside of a Western environment. What questions do you have after reviewing and reading? Are there any key points you would want to hear more about? Here are my top share worthy pieces of content I've stumbled across in the past week! This list is a little shorter than usual because (if you've been following along you know) I unplugged for a bit to do Disney World with my family. Now that I am getting myself back up to speed, here is what has caught my eye.
April was Alcohol Awareness Month - @neda did a great post sharing that about 20% of eating disorder patients develop an alcohol use disorder. This week at Digestive Disease Week I have also been learning about the correlation between IBD and developing an alcohol use disorder. This topic is very top of mind for me right now and I like that this post highlights some resources for those looking for support. May 4th was the first Terminated for Medical Reasons Awareness day. This topic is an emotional one and often hard to talk about, but with abortion rights continuing to diminish we need to be talking about this. @postpartumsupportinternational shared a powerful post about one mother's experience with TFMR and her explanation of why it is so critical to protect this right. NPR on Messy House Shame - My mom actually sent me this article because she knows how hard I stress over keeping my home together. This article provides some relief in validating that you are running your home just the way you are supposed to for your family. |
Blonde babe.
Millennial mom. Crohn's crusher. Mental health advocate. Sharing my raw and real journey through motherhood and navigating Crohn’s Disease. CrohnicallyBlonde is a place where I serve up my unfiltered commentary on chronic illness, mental health, pregnancy, and motherhood alongside lighter lifestyle content like beauty product reviews, travel tips, and book recommendations. My hope is that by authentically sharing my story I can help others going through similar situations not feel so alone and maybe even laugh along with me. categories
All
archives
November 2023
|
|
LET'S CONNECT ON SOCIAL
|
ContactFor press, partnerships, and general inquiries please contact: [email protected]
|










 RSS Feed
RSS Feed